Living with diabetes often means taking extra care when it comes to your health, and that includes your dental health, too. If you’ve been thinking about getting dental implants but are unsure whether it’s a safe option because of your diabetes, this blog is for you. It’s one of the most common concerns we hear from patients.
Diabetes doesn’t automatically rule out dental implants, but it does mean that your dentist needs to take a closer look at how to plan treatment safely and successfully.
In this post, we’ll walk through what you need to know about dental implants and diabetes, from potential risks to what makes someone a good candidate, so you can feel more confident about your next steps.
How Diabetes Can Affect Your Oral Health
Before we dive into implants specifically, it helps to understand how diabetes can impact your mouth. People with diabetes are more prone to:
- Gum disease (periodontal disease)
- Delayed healing after surgery
- Dry mouth
- Higher risk of infection
All of these can affect how your body responds to dental procedures, especially something like an implant, which requires the bone and gums to heal properly for long-term success.
But here’s the key point: well-controlled diabetes often doesn’t carry the same risks as poorly managed diabetes.
Are Dental Implants Safe If You Have Diabetes?
Yes, many people with diabetes can safely get dental implants, especially if their blood sugar is well-managed.
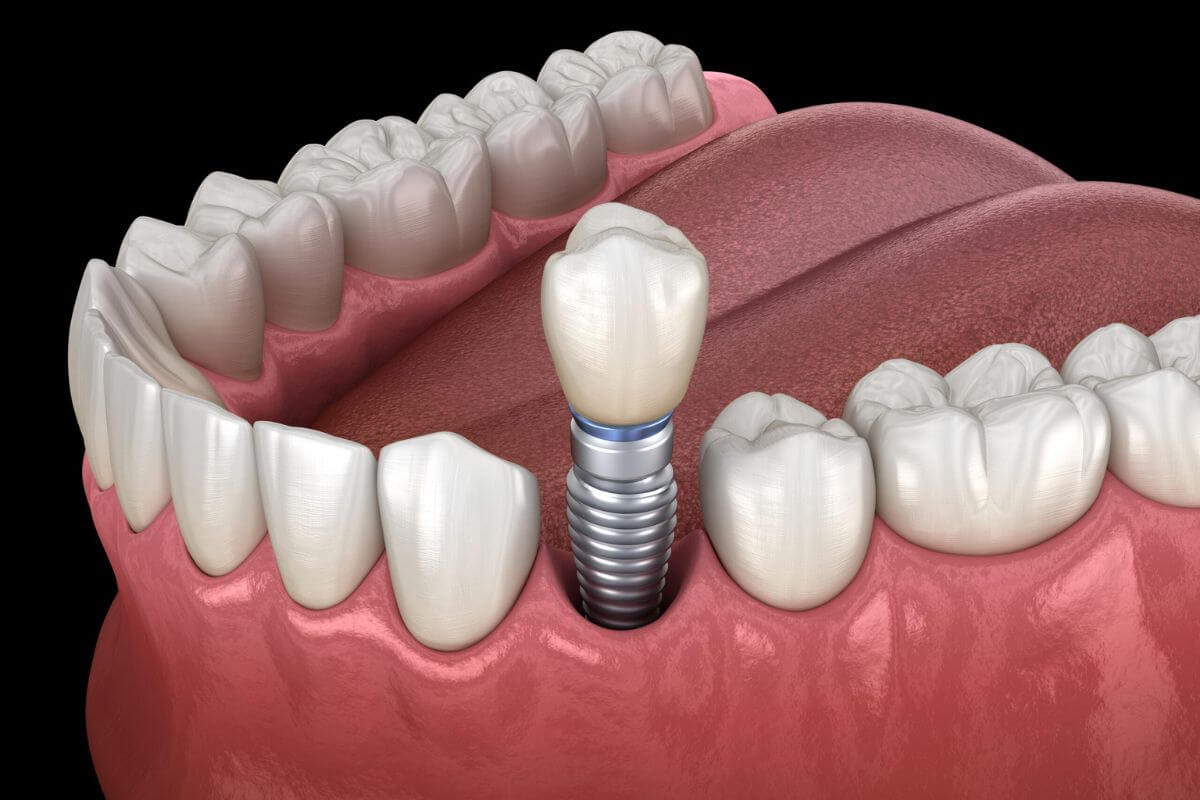
The main concern is how your body heals. Implants need time to fuse with the bone (a process called osseointegration), and poor healing can interfere with this. But studies have shown that patients with controlled diabetes have similar success rates to those without diabetes.
In other words, it’s not just whether you have diabetes, but how well it’s managed that matters most.
What Makes a Good Candidate for Dental Implants?
For individuals with diabetes considering dental implants, several factors are taken into account to determine candidacy:
- Blood sugar control: Ideally, A1C levels should be in a stable, healthy range to support proper healing.
- Gum health: Healthy gums help provide a strong foundation for implant placement.
- Bone density: There needs to be sufficient bone in the jaw to anchor the implant securely. This is usually assessed through X-rays or 3D imaging.
- No signs of active infection: The mouth should be free of gum disease or other ongoing oral health issues.
- Overall health and healing: Any medications, previous surgeries, or health conditions that might affect healing are typically reviewed as part of the planning process.
In some cases, coordination with a patient’s primary care provider or endocrinologist may also be helpful to ensure that diabetes is being managed in a way that supports safe and effective treatment.
What Happens If My Diabetes Isn’t Well-Controlled?
If your blood sugar levels are unpredictable or high, your dentist may recommend postponing implant surgery until they’re more stable.
In the meantime, you may be recommended other options to improve your oral health, like treating any gum issues or planning for bone support if needed. Sometimes even small steps now can open the door to implants down the line.
Why It’s Still Worth Considering Implants
For patients who qualify, implants are often the most natural-feeling and longest-lasting way to replace missing teeth. Compared to bridges or dentures, implants:
- Help prevent bone loss in the jaw
- Don’t rely on neighboring teeth for support
- Look and function like real teeth
- Can make eating and speaking feel more natural
That’s why so many patients with diabetes still choose implants, as they offer long-term benefits when done with care.
Preparing for Implant Treatment When You Have Diabetes
If diabetes is well-controlled and other oral health factors are in good shape, dental implants can often be placed successfully. The planning process may include a few additional steps compared to someone without diabetes.
Medical history and current health status are usually reviewed to assess how well the body is likely to heal after surgery. This can include looking at blood sugar trends, A1C levels, and any other medical conditions or medications that might affect recovery.
Gum and bone health are also important considerations. For some patients, periodontal treatment or bone grafting may be recommended before implant placement to ensure the best possible foundation.
Timing and healing expectations may be adjusted slightly as well. Healing can sometimes take longer in individuals with diabetes, so careful follow-up and monitoring are essential throughout the process.
By approaching treatment with these factors in mind, the risk of complications can be reduced, and long-term outcomes tend to be more predictable.
Thinking About Dental Implants? Start With a Consultation at Stonehaven Dental & Orthodontics in Waco
If you’re managing diabetes and wondering whether dental implants are right for you, the best place to start is with a personalized evaluation. We’ll answer your questions, check the health of your gums and jaw, and walk you through your options.
Contact us in Waco to schedule a consultation and find out if you’re a good candidate for dental implants.
Frequently Asked Questions
1. Can uncontrolled diabetes disqualify me from getting dental implants?
Uncontrolled diabetes doesn’t necessarily disqualify someone from getting implants, but it can increase the risk of complications such as delayed healing or infection. Most dental professionals will recommend stabilizing blood sugar levels before moving forward with implant surgery to improve the chances of a successful outcome.
2. Do people with diabetes take longer to heal after dental implant surgery?
Healing times can vary from person to person, but diabetes, if not well-managed, may slow the healing process. This is because high blood sugar can affect circulation and the body’s ability to repair tissue. With proper monitoring and good glycemic control, many patients heal within the expected timeframe.
3. Are there any extra precautions needed before or after implant surgery for diabetic patients?
Yes, additional precautions may include monitoring blood sugar levels closely before and after the procedure, ensuring any signs of gum disease are treated in advance, and possibly using antibiotics to reduce infection risk. Post-operative care and regular follow-up are also especially important to track healing progress.
4. Are dental implants better than dentures or bridges for people with diabetes?
Dental implants can offer more stability and comfort compared to removable dentures, and they help prevent bone loss in the jaw—a common issue after tooth loss. However, whether they’re the best option depends on individual health, bone condition, and how well diabetes is managed. A thorough evaluation can help determine the most suitable choice.